

Journal of Medical Sciences and Health
DOI: 10.46347/jmsh.v12.i1.25.383
Year: 2026, Volume: 12, Issue: 1, Pages: 60-66
Original Article
Latesh Raghute 1, Ishi Sharma 2, Minal Nagvekar 3, Sakshi Dandade 2, Pooja Ghadage 2, Abhijeet Mohite 4
1Associate Professor, Department of Pharmacology, GMC Sindhudurg, Maharashtra, India.
2Final MBBS student, GMC Sindhudurg, Maharashtra, India.
3Assistant Professor, Department of Obstetrics and Gynaecology, GMC Sindhudurg, Maharashtra, India.
4 Junior Resident, Department of Pharmacology, GMC Sindhudurg, Maharashtra, India.
Address for correspondence: Latesh Raghute, Associate Professor, Department of Pharmacology, GMC Sindhudurg, Maharashtra, India.
E-mail: [email protected]
Received Date:14 November 2025, Accepted Date:16 January 2026, Published Date:30 March 2026
Introduction: Menstruation is a normal biological process, yet it is surrounded by cultural taboos and misinformation. Lack of awareness and poor menstrual hygiene management (MHM) can lead to reproductive tract infections (RTIs), psychosocial issues and school absenteeism. Objectives: To assess knowledge and practices of menstrual hygiene among young school-going girls aged 12 -18 years in Sindhudurg district of Maharashtra and to determine their proportion about awareness and significance of menstrual hygiene practices. Materials and Methods: In this cross-sectional observational study, 284 girls from 7th to 12th grade who have attained menarche were selected by two-stage cluster sampling method. Data were collected using a predesigned and prevalidated questionnaire, with informed consent and assent, followed by a health education session. Statistical analysis was performed using MS Excel. Results: Mean age of participants was 15.05±1.20 years and mean age at menarche was 12.5±1.20 years. Prior awareness about menstruation before menarche was reported by 68%. Menstruation as physiological process was understood by 83%; while 10% girls believed menstruation was a curse. In hygiene practices: 96% used disposable sanitary pads, and 68% changed pads ≥ 3 times/day. Only 29% consistently used soap for genital cleaning. Disposable practices included burning (57%) and household garbage (43%). Eleven percent reported school absenteeism; while 64% had genital itchiness and 3.5% had RTIs. Conclusion: Awareness and hygiene practices were generally satisfactory, but gaps remain in early education, consistent hygiene, and safe waste disposable. Strengthening school-based health education, improving WASH facilities, and culturally sensitive programs are needed to ensure safe MHM.
Keywords: Menstrual hygiene management, School absenteeism, WASH facilities, Sindhudurg
Menstruation is the visible manifestation of cyclical, physiological uterine bleeding due to shedding of the endometrium[1]. It starts during puberty and stops permanently at menopause[2]. The first menstruation –menarche- occurs between 9 years and 16 years. Menstruation is the physiological process in a girl’s body and is an indication of normal growth and development[3]. In recent years, a trend toward earlier
onset of menarche has been observed, sometimes as early as nine years. Therefore, sympathetic guidance and appropriate support for young girls experiencing menstruation are of paramount importance. Even though menstruation is a normal biological process, it is surrounded by cultural taboos and misinformation in many communities. Also, lack of awareness and poor menstrual hygiene can lead to health problems like reproductive tract infections (RTIs) and social consequences such as school absenteeism[4]. Inadequate menstrual hygiene management (MHM) practices among adolescent girls in underdeveloped and developing nations continue to pose challenges for girls themselves, their families, broader society and public health authorities. Menstruation related problems are widespread among adolescent girls in India. Menstrual abnormalities and disorders are frequently linked to physical, mental, social, psychological and reproductive issues[5].
Research has shown that there is a strong association between practices during menstruation and prevalence (reported symptoms) of RTIs. The prevalence of RTIs was more than 3 times higher among girls having unsafe and unhygienic menstrual practices[6] and various surveys suggest that poor management results absenteeism in school, distraction in studies and disengagement in other activities[7]. Effective MHM is vital to enable women and girls to participate in daily life with dignity, comfort and confidence[8]. It encompasses Hardware intervention which includes the provision of absorbents or improved water sanitation and Software interventions which address deficit in knowledge of menstruation and management by providing education[9]. According to a study, although initially only 34% girls were aware that menstruation is a normal process, the number increased to 80% after giving them health education[10]. This observation highlights the importance of Health Education Programs in schools focusing mainly on menstrual hygiene and reproductive health among both adolescent girls and boys.
Thus, the present study aims to assess the awareness and practices related to menstrual hygiene among school going-girls aged 12-18 years in Sindghudurg district, Maharashtra. The findings are expected to identify existing knowledge gaps, behavioural patterns and their implications for health and education, thereby informing strategies for improved MHM in school settings.
To assess the knowledge and practices of menstrual hygiene among young school-going girls aged 12 -18 years in Sindhudurg district of Maharashtra.
To determine the proportion of young girls aware about the significance of menstrual hygiene practices.
Study design: A cross-sectional observational study.
Ethical approval: The study was approved by the Institutional Ethics Committee.
Study population: This study was conducted among the young school going girls from 7th to 12th grade mainly in the age group 12-18 years attending government or private schools in Sindhudurg district of Maharashtra, who have attained menarche and who are willing to participate in the study.
Inclusion criteria
Young school-going girls mainly in the age group 12-18 years who have achieved the menarche.
Girls who are comfortable sharing their menstrual practices and habits and are willing to participate in the study.
Girls from 7th to 12th standard attending the school as per allowance and consent by the School Principal.
Exclusion criteria
Girls below 12 years of age and above 18 years of age will not be included.
Girls who are not willing to participate voluntarily in the study.
Girls who are not attending the school.
Sampling procedure
A two-stage cluster sampling method was employed: First, the accessible schools (both government and private) in Sindhudurg district were selected by simple random sampling and then the eligible girls (aged 12–18 years who have attained menarche) within selected schools were chosen by simple random sampling from class lists.
Sample size
As per one study [11], taking the prevalence rate of satisfactory menstrual hygiene practices to be 80%, using the formula Z²P(1 -P)/D² with 95% confidence limit, 5% absolute error, and 10% non -responsive rate, the sample size came to be 284.
Data Collection
After obtaining permission from the principal and with the consensus of class teacher, time and date of data collection was planned accordingly. Informed consent was obtained via school authorities and assent from participants. Data was gathered using a predesigned and prevalidated questionnaire that included questions about menstrual awareness. Each interview was started with greetings and explanation of the questionnaire which was made available in both Marathi and English (or regional language when required). All the data collected were kept fully anonymous and privacy was maintained while conducting the interviews. A health education session was also conducted on menstrual hygiene and its significance after collecting the data from the required participants. Data of all the participants was kept confidential.
Statistical analysis
The collected data from the interview was entered in an Excel sheet and analysis was done using MS Excel software. For continuous variables like age, mean with standard deviation was calculated. Categorical data like menstrual material used, frequency of changing menstrual material used, and place of disposal of material at home was presented as proportion.
Study duration
Three months (From November 2024 to January 2025).
A total of 284 girls participated in the study. [Table. 1] shows distribution of participants by age and grade. The Mean age of participants was 15.05±1.20 years (range 12–18) and the mean age at first menstruation was 12.5±1.20 years (range 12–18). Most of the participants (83.8 %) were from grade eight, nine and ten. Almost 99 % girls have someone (either mother, female relative or friend) whom they would feel comfortable asking for support regarding menstruation.
| Sr. No. | Variable | Category | Frequency (n = 284) |
Percentage (%) |
|---|---|---|---|---|
| 1 | Age (years) | 12-13 | 24 | 8.5 |
| 14-15 | 163 | 57.4 | ||
| 16-18 | 97 | 34.1 | ||
| 2 | Grade | 8th – 10th | 238 | 83.8 |
| 11th -12th | 46 | 16.2 |
As per [Table. 2], showing knowledge about menstruation among participants, significant number of girls (32%) had not received any information about menstruation before menarche, meaning roughly one-third were unprepared at first period (68% had prior knowledge). 83% understood the physiological reason for menstruation, while 17% did not. School-based education was high: 96.5% reported being taught appropriately about menstrual hygiene in school, and 95% had been taught about menstruation at home. About 10% girls believed menstruation was a curse or that menstrual blood was impure, while 90% disagreed. Only 72% correctly identified the vagina as the source of menstrual blood; 24% said “don’t know” and 4% incorrectly said “urethra.” This indicates about a quarter of girls had confusion about basic menstrual physiology.
| Sr. No. | Knowledge Aspect | Response (Yes) |
Response (No) |
|---|---|---|---|
| 1 | Heard of menstruation before menarche | 193 (68.0 %) | 91 (32 %) |
| 2 | Knew menstruation is physiological | 235 (82.7 %) | 49 (17.3 %) |
| 3 | Belief that menstruation is curse and that blood is impure | 28 (9.9 %) | 256 (90.1 %) |
| 4 | Knowledge about menstrual blood comes from and source | 205 (72.2 %) | 79 (27.8 %) |
[Table. 3] shows hygiene practices during menstruation among participants. Nearly all girls (96.1%, 273/284) used disposable sanitary pads; only 1.1% used cloths, 1.8% reusable pads, and 1.1% absorbent underwear. When asked what they would prefer if given an option, 85% chose single-use pads, 6% menstrual cups, 3.5% reusable pads, 6% absorbent underwear, and the remainder “other”. During their last period, the number of pad changes per day was mostly ≥ 3 times/day (68.3 %), meeting recommended hygiene frequency while 27.5 % reported twice and 4.2 % reported one time a day. Hygienic bathing and cleaning were common: 100% reported bathing during menstruation, with 47% washing genitals ≥3 times per day and 32% twice per day. Hand washing with soap before/after handling menstrual material was nearly universal (283/284, 99.6%). However, soap use on genitals was lacking: 40% never used soap on genital wash, 31% sometimes, and only 29% always did so. Thus, a substantial proportion did not regularly clean with soap, which could pose infection risks.
Disposal of used pads was mostly done by burning (57% of girls). Others disposed in household garbage either into a latrine toilet bin (25%) or outside bin (18%). Only 2% reported disposing pads without wrapping; 98% wrapped pads (mainly in paper (66%) or plastic (27%)). Among girls who reused cloth and absorbent underwear (n≈6), 73% soaked/wash with soap and 75% always sun-dried or ironed them for sterilization.
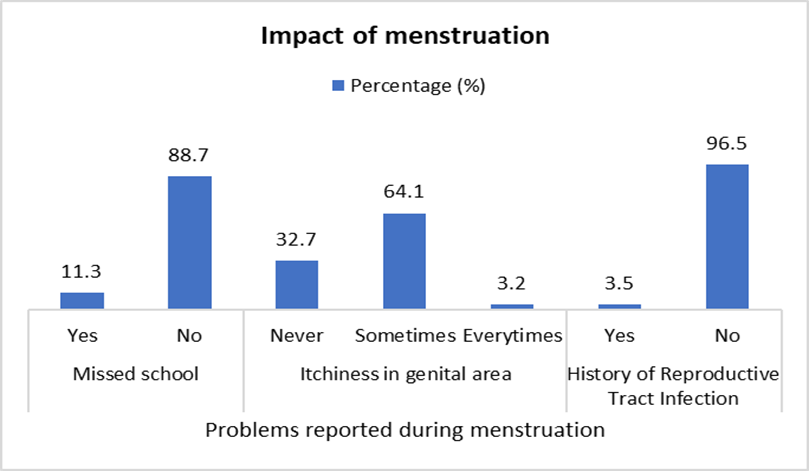
According to [Fig. 1], school absenteeism was reported by 11% of girls (32/284) who often missed school during menstruation; 89% never missed. Those missing school primarily cited discomfort or lack of facilities. Despite overall good school education on menstruation, any absenteeism highlights remaining barriers. About 64% reported genital itchiness during periods (mostly “sometimes”), and 3.5% reported a history of reproductive tract infection (RTI); 96.5% had never had an RTI.
| Sr. No. | Practice | Category | Frequency (n = 284) |
Percentage (%) |
|---|---|---|---|---|
| 1 | Type of absorbent used | Single Use pad / Sanitary Napkin | 273 | 96.1 |
| Reusable sanitary pad | 5 | 1.8 | ||
| Absorbent underwear | 3 | 1.1 | ||
| Cloth | 3 | 1.1 | ||
| 2 | Frequency of absorbent change | One time a day | 12 | 4.2 |
| Two times a day | 78 | 27.5 | ||
| ≥ Three times a day | 194 | 68.3 | ||
| 3 | Washing of genitals during menstrual period | At the end of menstrual period only | 5 | 1.8 |
| Every 2-3 days | 11 | 3.9 | ||
| One time a day | 42 | 14.8 | ||
| Two times a day | 92 | 32.4 | ||
| ≥ Three times a day | 134 | 47.2 | ||
| 4 | Disposal of menstrual material | Burned | 161 | 56.7 |
| Household garbage | 123 | 43.3 |
This study was carried out to assess the awareness and practices related to menstrual hygiene among 284 young school-going girls aged 12-18 years in Sindhudurg district, Maharashtra. The mean age of the participants was 15.05±1.20 years (range 12-18) and the mean age at first menstruation was 12.5±1.20 years (range 12-18). In our study, 68% of participants had heard of menstruation before experiencing menarche. This finding is similar with studies carried out by Sarangi S et al. in Delhi (70%) and Kaliappan I et al. in Coimbatore (65%) [12, 13]. This proportion also parallels international data from Kenya (72.8%) and Nepal (66%)[14, 15]. The existence of prior knowledge suggests that awareness programs and peer discussion may be reaching a significant proportion of girls. However, the finding that 32% participants were unaware prior to menarche highlights the continuing gaps in early reproductive health education. Insufficient knowledge before the onset of menstruation can
contribute to the feelings of anxiety, fear and confusion, often leading to negative psychological experiences during menarche. Implementing early, age-appropriate reproductive health education ideally integrated within school curricula and community based programs can help normalize menstruation as a natural physiological process rather than a source of shame or embarrassment. In this study, 83% of participants correctly recognised menstruation as a physiological and natural process. These findings are in line with previous Indian studies conducted in West Bengal (86%) and Maharashtra (71%) and comparable with study from Ethiopia (78%) [16-18]. These findings suggest that school-based education and media have played a helpful role in spreading awareness about menstruation.
Regarding myths and misconceptions, only 10% of participants believed that menstruation to be a curse or that menstrual blood was impure comparable to sub-Saharan Africa (8-14%)[19]. While the study carried out by Lonimath A et al. found that 27.4% of girls believed menstrual blood was impure[20]. These findings suggest a gradual cultural transition towards greater menstrual awareness; however strong social stigma still makes it hard to talk openly and learn about it. About 72% girls correctly identified the vagina as the outlet of menstrual blood, similar to findings from urban Indian schools (70-75%) and Ghana (68%)[21, 122]. Despite this, confusion persisted among 28%, revealing partial understanding of reproductive anatomy.
A remarkably high proportion (96%) of respondents reported using disposable sanitary pads, similar to rates reported from urban India (92-97%) and Ghana (96%)[12, 13, 23]. This contrasts with rural Indian data where usage remains between 60-70% and with Nigerian findings showing 88%[17, 24]. This disparity reflects the role of socioeconomic status, accessibility and awareness. About 68% of participants changed pads ≥3 times/day, meeting CDC-recommended hygiene standards[25]. These findings are consistent with findings from Delhi (65%) and Maharashtra (63.3%)[12, 26]. Frequent pad changes prevent microbial growth and infection, contributing to reproductive tract health. However the remaining 32% changing pads less frequently may face risks of infection and discomfort, emphasizing the need to reinforce hygiene practices through school health programs. Nearly half (47%) washed genitals ≥3 times/day, aligning with studies by Kadpatti MG et al. (46%) and Hussein J et al. (48%)[27, 28]. However, only 29% reported using soap consistently, which is concerning as poor genital hygiene can predispose individuals to infections. A study by Adhikari P et al. from Nepal (11%) further supports this challenge[15]. Barriers may include limited privacy, water availability and lack of awareness about proper washing techniques. Hence MHM programs must not only emphasize frequency but also quality of hygiene practices.
Burning was the most common method of sanitary pad disposal (57%) consistent with finding from rural India (61%), followed by disposal in household garbage (43%), similar to Gupta et al. (37%)[17, 29]. Although prevalent, these practices raise environmental concerns due to emissions from open burning and inadequate waste handling. None of the participants reported disposing of pads into latrine pits which is positive finding, as such practices can obstructs drainage systems and pose environmental risks. In contrast, other studies have reported latrine disposal leading to drainage blockages[18, 22, 23]. Establishing incinerators in schools and community facilities can promote safe, hygienic and environmentally sustainable menstrual waste management.
Menstrual-related school absenteeism was reported by 11% of participants, aligning with findings from various other studies[16, 23, 29]. The main causes included discomfort, poor sanitation and fear of staining and teasing. Such absenteeism hinders academic performance and reinforces gender disparities in education. Establishing menstrual-friendly schools with adequate water, sanitation and disposal facilities, along with teacher sensitization, can greatly improve girls attendance and confidence during menstruation.
About 64% of girls reported genital itchiness and 3.5% had symptoms of RTI, consistent with study by Mathiyalagen P et al. linking poor hygiene to such issues[30]. Infections during adolescence can impact future reproductive health, highlighting the life-course approach that early hygiene practices shape long term well-being. Preventive education during adolescence is therefore crucial for sustaining reproductive health.
The majority adolescent school-going girls in our cross-sectional study demonstrated satisfactory awareness and hygienic practices regarding menstruation, still significant gaps remain in knowledge of reproductive physiology and consistent hygienic behaviours. Nearly one-third of participants were unaware of menstruation before menarche, and misconceptions such as perceiving menstruation as curse persisted among a minority. Even though almost everyone used disposable sanitary pads, it was reported that some participants didn’t change their pads often enough and didn’t clean their genital properly. School absenteeism, while comparatively low, highlights the persistent challenges presented by discomfort and insufficient facilities. These findings emphasize the importance of strengthening school-based health education, improving WASH infrastructure, installing pad disposing machines under government programs and promoting culturally sensitive awareness programs to ensure safe and dignified menstrual hygiene management for adolescent girls.
The data were self-reported, which may be affected by recall or social desirability bias, particularly for culturally sensitive topics. As the research was confined to a single district, the findings may not fully represent areas with different sociocultural settings. Moreover, the use of structured questionnaire limited the ability to explore deeper insides into attitudes, beliefs and stigma surrounding menstruation.
Funding: No funding sources.
Conflict of interest: None declared.
1. Chakravorty BN, Dutta DC. Menstruation. In: Konar H, editor. <I>DC Dutta’s textbook of gynecology: including contraception</I>. 6th ed. New Delhi: Jaypee Brothers Medical Publishers (P) Ltd; 2014. p. 82–98.
2. Merck Manual Consumer Version. <I>Menstrual Cycle</I>. Rahway (NJ): Merck & Co., Inc. Available from: https://www.merckmanuals.com/home/women-s-health-issues/biology-of-the-female-reproductive-system/menstrual-cycle.
3. Ministry of Health and Family Welfare. <I>Flipbook on Menstrual Hygiene</I>. New Delhi: National Health Mission; [cited 2025 Oct 15]. Available from: https://nhm.gov.in/images/pdf/programmes/mhs/Training_Materials/PDF_English/flipbook.pdf.
4. Menstrual hygiene practices and associated factors among Indian adolescent girls: a meta-analysis. Reproductive Health. 2022; 19 (1). Available from: https://doi.org/10.1186/s12978-022-01453-3
5. Menstrual hygiene practices among adolescent girls in a resettlement colony of Delhi: a cross-sectional study. International Journal of Reproduction, Contraception, Obstetrics and Gynecology. 2017; 6 (5). Available from: https://doi.org/10.18203/2320-1770.ijrcog20171954
6. Menstrual Practices and Reproductive Problems. Journal of Health Management. 2005; 7 (1). Available from: https://doi.org/10.1177/097206340400700103
7. Poor management of menstrual hygiene: a leading cause of school absenteeism among adolescent girls in the urban slum of Madhya Pradesh. International Journal of Reproduction, Contraception, Obstetrics and Gynecology. 2020; 9 (10). Available from: https://doi.org/10.18203/2320-1770.ijrcog20204295
8. Ministry of Drinking Water and Sanitation. Menstrual Hygiene Management: National Guidelines. 2015;(December):36. Available from: https://swachhbharatmission.ddws.gov.in/sites/default/files/Guidelines/Menstrual-Hygiene-Management-Guidelines.pdf
9. Do Menstrual Hygiene Management Interventions Improve Education and Psychosocial Outcomes for Women and Girls in Low and Middle Income Countries? A Systematic Review. PLOS ONE. 2016; 11 (2). Available from: https://doi.org/10.1371/journal.pone.0146985
10. Dorle AS, Gavel S, Mannapur BS MR. Impact of health education on knowledge and practices about menstruation among college-going adolescent girls. <I>Medica Innovatica</I>. 2019;8(2):21–5. https://medicainnovatica.org/Medicajan2020/IndartMed%20InnDec%202019/Article%205.pdf
11. Prevalence of hygiene awareness during menstruation period among rural women of West Bengal, India. International Journal Of Community Medicine And Public Health. 2024; 11 (2). Available from: https://doi.org/10.18203/2394-6040.ijcmph20240273
12. A Comparative Study of Menstrual Hygiene Knowledge and Practices among International and Government School going Adolescent Girls in Delhi. International Journal of Current Research and Review. 2024; 16 (20). Available from: https://doi.org/10.31782/ijcrr.2024.162001
13. Knowledge, attitude, and practice on menstrual hygiene among adolescent girls in Coimbatore: A cross-sectional study. World Journal of Biology Pharmacy and Health Sciences. 2025; 21 (1). Available from: https://doi.org/10.30574/wjbphs.2025.21.1.0012
14. Menstrual hygiene management practices among primary school girls from a pastoralist community in Kenya: a cross sectional survey. Pan African Medical Journal. 2018; 31 Available from: https://doi.org/10.11604/pamj.2018.31.222.13521
15. Adhikari P, Kadel B, Dhungel SI, Mandal A. Knowledge and practice regarding menstrual hygiene in rural adolescent girls of Nepal. <I>Kathmandu University Medical Journal</I>. 2007;5(19):382–6. https://pubmed.ncbi.nlm.nih.gov/18604059/
16. Menstrual hygiene: How hygienic is the adolescent girl?. Indian Journal of Community Medicine. 2008; 33 (2). Available from: https://doi.org/10.4103/0970-0218.40872
17. Thakre SB, Thakre SS, Reddy M, Rathi N, Pathak K, Ughade S. Menstrual hygiene: Knowledge and practice among adolescent school girls of Saoner, Nagpur District. <I>Journal of Clinical and Diagnostic Research</I>. 2011;5(5):1027–33. https://www.ircwash.org/sites/default/files/Thakre-2011-Menstrual.pdf
18. Menstrual hygiene management and school absenteeism among female adolescent students in Northeast Ethiopia. BMC Public Health. 2014; 14 (1). Available from: https://doi.org/10.1186/1471-2458-14-1118
19. Comfortably, Safely, and Without Shame: Defining Menstrual Hygiene Management as a Public Health Issue. American Journal of Public Health. 2015; 105 (7). Available from: https://doi.org/10.2105/ajph.2014.302525
20. Effect of health education on knowledge and beliefs about menstruation among adolescent girls studying in a tribal school of Mysore – A quasi-experimental study. RGUHS National Journal of Public Health. 2017; 2 (4). Available from: https://doi.org/10.26463/rnjph.2_4_2
21. Menstrual hygiene management among adolescent girls in India: a systematic review and meta-analysis. BMJ Open. 2016; 6 (3). Available from: https://doi.org/10.1136/bmjopen-2015-010290
22. Menstrual Hygiene Management and School Absenteeism among Adolescents in Ghana: Results from a School-Based Cross-Sectional Study in a Rural Community. International Journal of Reproductive Medicine. 2020; 2020 Available from: https://doi.org/10.1155/2020/6872491
23. Menstrual Hygiene Knowledge, Practices and Interventions Among Junior High School Girls in the Krobo Area of Ghana. Journal of Environment and Sustainable Development. 2023; 2 (1). Available from: https://doi.org/10.55921/fosd3466
24. Lawan UM, Yusuf NW, Musa AB. Menstruation and menstrual hygiene amongst adolescent school girls in Kano, Northwestern Nigeria. <I>African Journal of Reproductive Health</I>. 2010;14(3):201–7. https://pubmed.ncbi.nlm.nih.gov/21495614/
25. Centers for Disease Control and Prevention. <I>Healthy Habits: Menstrual Hygiene</I>. Available from: https://www.cdc.gov/hygiene/about/menstrual-hygiene.html.
26. Menstrual hygiene among adolescent girls – A study from urban slum area. Journal of Family Medicine and Primary Care. 2018; 7 (6). Available from: https://doi.org/10.4103/jfmpc.jfmpc_80_18
27. Kadapatti MG, Genevieve KH. Menstrual Hygiene Practices Followed among Rural Adolescent Girl Students. <I>International Journal of Health Sciences and Research</I>. 2024;14(9):35–43. https://jiaap.in/menstrual-hygiene-practices-followed-among-rural-adolescent-girl-students/
28. The practice of menstrual hygiene management and associated factors among secondary school girls in eastern Ethiopia: The need for water, sanitation, and hygiene support. Women's Health. 2022; 18 Available from: https://doi.org/10.1177/17455057221087871
29. A cross-sectional study on menstrual hygiene practices among school going adolescent girls (10-19 years) of Government Girls Inter College, Saifai, Etawah. International Journal Of Community Medicine And Public Health. 2018; 5 (10). Available from: https://doi.org/10.18203/2394-6040.ijcmph20184010
30. A descriptive cross-sectional study on menstrual hygiene and perceived reproductive morbidity among adolescent girls in a union territory, India. Journal of Family Medicine and Primary Care. 2017; 6 (2). Available from: https://doi.org/10.4103/2249-4863.220031
Subscribe now for latest articles and news.